How to Set Up a Telemedicine Program in a Nursing Home: Step-by-Step Guide
Step 1: Assess Your Clinical Needs and Current Infrastructure
Nursing home residents need immediate access to medical specialists. Your facility averages 3.2 emergency room visits per resident annually. Half could be prevented with proper remote consultation capabilities.
The challenge isn't just finding doctors willing to provide teleconsultations. It's building a clinical workflow that actually works during a medical crisis at 2 AM when your charge nurse needs cardiology input and can't wait for morning rounds.
Start with your most frequent specialist referrals. Pull your last 12 months of data. Which specialties do you call most often? Cardiology, pulmonology, and psychiatry typically top the list for most facilities.
Document your current process for urgent consultations. How long does it take to reach a specialist? What happens during evenings and weekends? Map out the actual workflow your nurses follow when they need clinical input.
Evaluate your existing technology infrastructure:
Internet connectivity: You need minimum 2 Mbps upload speed per concurrent consultation. Test your bandwidth during peak hours, not just during quiet periods.
Hardware inventory: Count available tablets, computers, and mobile devices. Note their age and operating system compatibility.
Staff comfort with technology: Survey your nursing staff honestly. A 68-year-old charge nurse with 30 years of experience brings clinical wisdom but may need additional technology training.
Physical space considerations: Identify quiet areas suitable for video consultations. Patient rooms work, but you also need spaces for family conferences and sensitive discussions.
Step 2: Define Your Program Goals and Scope
Set specific, measurable objectives for your telemedicine program. Avoid vague goals like "improve patient care." Instead, target concrete outcomes:
- Reduce emergency department transfers by 25% within 6 months
- Achieve specialist consultation within 30 minutes for urgent cases
- Decrease average length of stay for respiratory infections by 2 days
- Maintain patient satisfaction scores above 90% for telehealth encounters
Determine which services you'll offer initially. Most successful nursing home programs start with:
Urgent consultation services: Cardiology for chest pain and arrhythmias, pulmonology for respiratory distress, psychiatry for behavioral emergencies.
Routine specialist follow-ups: Endocrinology for diabetes management, nephrology for chronic kidney disease, wound care specialists.
Primary care coverage: After-hours physician coverage, medication adjustments, acute illness management.
Choose your patient population carefully. Start with residents who can participate in video calls and have family members available for support. Expand to patients with dementia once your staff gains confidence with the technology.
Step 3: Select Your Technology Platform and Medical Devices
Your telemedicine platform needs to handle more than video calls. During a cardiac emergency, you need ECG data streaming live to the cardiologist while maintaining the video connection. The specialist needs to see the rhythm strip in real-time, not receive a faxed copy 20 minutes later.
Essential platform features:
- HIPAA-compliant video conferencing with recording capabilities
- Integration with your existing electronic health records
- Medical device connectivity for vital signs, ECG, and digital stethoscope
- Mobile compatibility for nursing staff
- 24/7 technical support
Medical device requirements:
Choose devices that integrate directly with your telemedicine platform. Standalone devices that require separate apps create workflow disruptions during emergencies.
Digital stethoscope: Essential for respiratory and cardiac assessments. Look for devices that transmit audio in real-time during video calls.
12-lead ECG capability: Critical for chest pain evaluation and arrhythmia assessment. The ECG should auto-upload to the patient record within 5 seconds.
Vital signs monitor: Blood pressure, pulse oximetry, and temperature measurement with automatic data capture.
Mobile cart or portable kit: Your nursing staff needs mobility. A cart works for planned consultations, but you also need portable equipment for bedside emergencies.
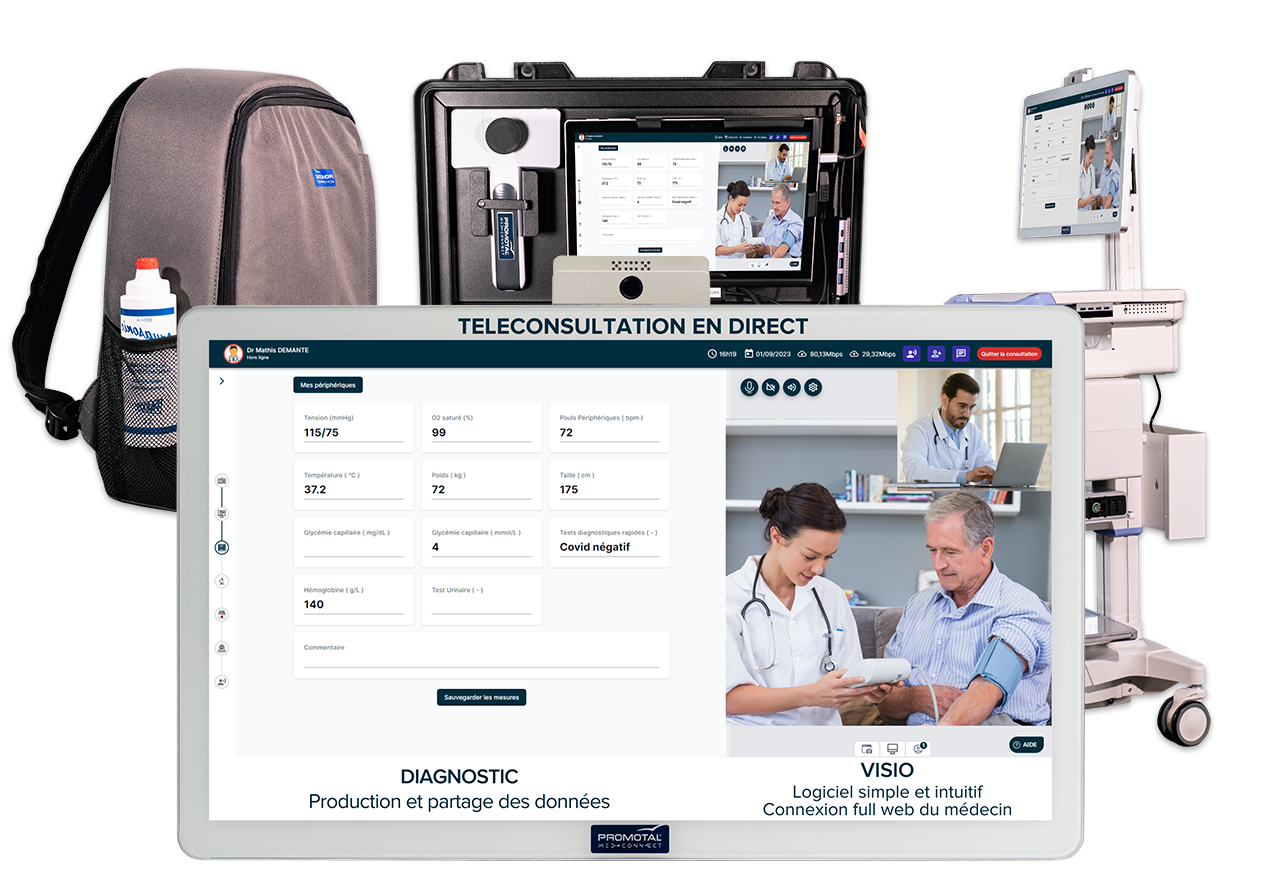
Platforms like MedConnect integrate all these components into a single clinical workflow. The ECG streams live to the remote physician while the consultation video continues uninterrupted. No toggling between apps during patient care.
Step 4: Ensure Regulatory Compliance and Documentation
Telemedicine in nursing homes requires strict adherence to multiple regulatory frameworks. Your state health department, CMS, and accreditation bodies all have specific requirements.
HIPAA compliance essentials:
- End-to-end encryption for all video and data transmission
- Secure storage of consultation recordings
- Staff training on privacy protocols during video calls
- Business associate agreements with all technology vendors
State licensing verification: Confirm that remote physicians hold valid licenses in your state. Some states have reciprocity agreements, others require full licensing.
Documentation requirements:
Every telemedicine encounter needs proper documentation in the patient record. Include:
- Date, time, and duration of consultation
- Participating healthcare providers
- Clinical findings and recommendations
- Any diagnostic data transmitted (ECG, vital signs)
- Follow-up care plan
Consent processes: Develop clear consent procedures for telemedicine services. Patients and families need to understand how the technology works and their rights regarding recorded consultations.
Quality assurance protocols: Establish regular review of telemedicine encounters. Monitor clinical outcomes, patient satisfaction, and technical performance.
Step 5: Develop Staff Training Programs
Your nursing staff determines program success. They need confidence with the technology and clear protocols for different clinical scenarios.
Technical training components:
- Platform navigation and basic troubleshooting
- Medical device operation and data transmission
- Audio and video quality optimization
- Emergency backup procedures when technology fails
Clinical workflow training:
Create specific protocols for common scenarios:
Chest pain protocol: Obtain 12-lead ECG, connect digital stethoscope, gather medication list, prepare for potential transfer orders.
Respiratory distress protocol: Check oxygen saturation, lung sounds via digital stethoscope, recent chest X-ray availability, current respiratory treatments.
Behavioral emergency protocol: Ensure patient and staff safety, gather recent medication changes, family contact information, previous psychiatric history.
Ongoing education requirements:
Schedule monthly competency assessments for the first six months. Focus on real scenarios, not just technology demonstrations. Your night shift staff need the same training intensity as day shift personnel.
Step 6: Establish Specialist Networks and Scheduling
Building relationships with remote specialists requires more than posting job listings. Specialists need to understand your facility's patient population and clinical capabilities.
Recruitment strategies:
Target specialists with nursing home experience. They understand the unique challenges of caring for elderly patients with multiple comorbidities.
Offer competitive compensation structures. Many specialists prefer per-consultation fees rather than hourly rates.
Scheduling and availability:
Establish clear coverage schedules for urgent consultations. Your residents can't wait until Monday morning for weekend chest pain evaluation.
Create escalation protocols when primary specialists are unavailable. Have backup coverage arrangements for each specialty.
Communication protocols:
Define when to use telemedicine versus phone consultation versus in-person visits. Not every clinical question requires video consultation.
Establish response time expectations: immediate for emergencies, within 2 hours for urgent issues, same-day for routine consultations.
Step 7: Implement Quality Monitoring and Continuous Improvement
Track specific metrics that matter for nursing home operations:
Clinical outcomes:
- Emergency department transfer rates before and after implementation
- Length of stay for common conditions
- Medication adjustment turnaround times
- Specialist referral completion rates
Operational metrics:
- Average time to specialist consultation
- Technology downtime incidents
- Staff satisfaction with telemedicine workflows
- Patient and family satisfaction scores
Financial impact:
- Cost per consultation versus traditional specialist visits
- Reduced transportation expenses
- Avoided emergency department charges
- Staff overtime reduction from faster clinical decision-making
Regular program review:
Conduct monthly reviews with nursing leadership, medical director, and participating specialists. Address technical issues immediately and clinical workflow problems within 48 hours.
Step 8: Scale and Expand Your Program
Start with one nursing unit or specific patient population. Prove the concept works before facility-wide deployment.
Expansion considerations:
Add specialty services based on demonstrated need and successful pilot results. Don't try to launch every specialty simultaneously.
Consider extending telemedicine to family communications. Remote family conferences reduce travel burden and increase participation.
Explore partnerships with other nursing homes for specialist sharing. A regional cardiology program can serve multiple facilities more efficiently.
Technology upgrades:
Plan for regular hardware replacement cycles. Medical devices and mobile equipment need replacement every 3-5 years.
Stay current with platform updates and new feature releases. Telemedicine technology evolves rapidly.
Consider integration with remote patient monitoring for chronic disease management. Continuous vital sign monitoring can trigger early specialist intervention.
Common Implementation Challenges and Solutions
Staff resistance to technology: Address concerns directly through hands-on training and peer mentoring. Pair technology-comfortable staff with those needing additional support.
Internet connectivity issues: Invest in redundant internet connections. Your telemedicine program can't depend on a single internet service provider.
Specialist availability: Develop relationships with multiple providers in each specialty. Single-provider arrangements create coverage gaps.
Patient and family acceptance: Start with families already comfortable with video calling. Success stories from early adopters encourage broader participation.
Regulatory compliance complexity: Work with healthcare attorneys familiar with telemedicine regulations. Requirements change frequently and vary by state.
Building a Sustainable Telemedicine Program
Successful nursing home telemedicine programs require ongoing commitment from administration, clinical staff, and technology partners. The initial investment in training and equipment pays dividends through reduced emergency transfers, faster clinical decision-making, and improved patient outcomes.
Your residents deserve access to specialist care without the trauma of unnecessary hospital transfers. A well-implemented telemedicine program provides that access while maintaining the clinical standards your facility demands.
The key is choosing technology that integrates into your existing clinical workflows rather than creating additional steps for your nursing staff. When the ECG automatically uploads to the patient record while the cardiologist reviews the rhythm in real-time, you've achieved true clinical integration.
Learn more at promotal-medconnect.com
Ready to discover MedConnect?
Request a personalized demo and see how the platform adapts to your practice.
Request a demo