What Is Clinical Teleconsultation? A Complete Guide for Healthcare Providers
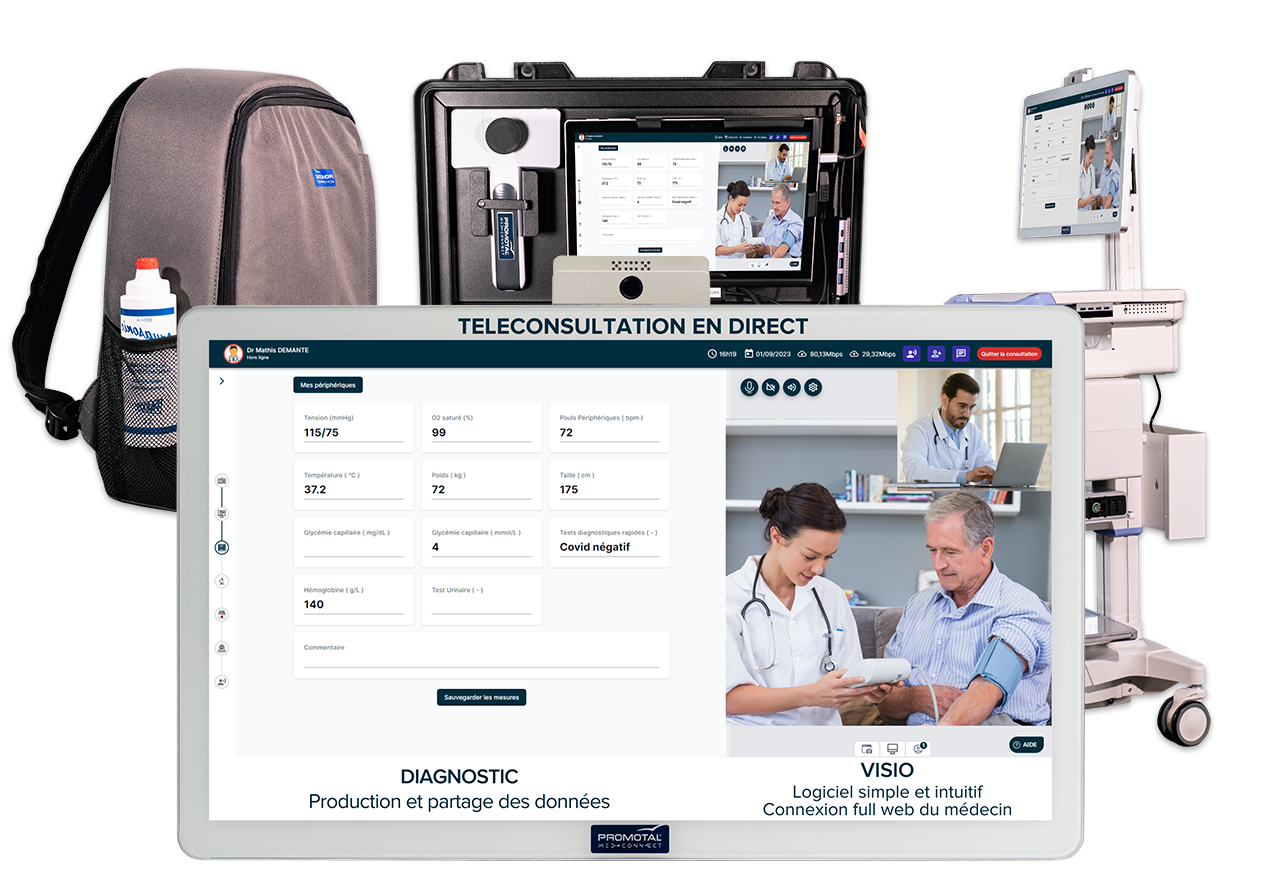
When a Video Call Is Not Enough
A patient at a rural clinic presents with chest pain. The nurse on-site can see them, but the nearest cardiologist is two hours away. A standard video call lets the remote doctor see the patient's face and hear their concerns — but it doesn't let them listen to the heart, read an ECG, or document findings directly into the patient record. Without those capabilities, you're left with a chain of manual steps that introduces delay, transcription errors, and real clinical risk.
That gap is exactly what clinical teleconsultation is designed to close.
This guide explains what clinical teleconsultation actually means, how it differs from a basic telemedicine video call, what a proper platform needs to handle, and what healthcare providers should be asking when they evaluate their options.
What Clinical Teleconsultation Actually Means
In the broadest sense, teleconsultation means any consultation conducted remotely using telecommunications technology. But that definition covers everything from a phone call to a fully integrated clinical workflow — and the distance between those two extremes is enormous.
Clinical teleconsultation is the structured, medically valid version. It replicates the diagnostic value of an in-person consultation as closely as possible, combining real-time data capture from clinical devices, secure video communication, and documented clinical reasoning. The output is a proper clinical encounter: a patient record, a SOAP note, a diagnosis or referral, and a billing event.
The word "clinical" is doing real work in that phrase. It means the consultation produces defensible, documented findings — not just a conversation.
How It Differs from Basic Telemedicine
Telemedicine is the umbrella. Clinical teleconsultation is a specific, higher-standard category within it.
| Feature | Basic Video Telemedicine | Clinical Teleconsultation |
|---|---|---|
| Video communication | ✓ | ✓ |
| Live clinical device data (ECG, stethoscope) | ✗ | ✓ |
| Automatic upload to patient record | ✗ | ✓ |
| Structured clinical documentation (SOAP) | Manual or absent | Auto-generated |
| Specialist referral workflow | External | Integrated |
| Billing integration | Separate | Built-in |
| Regulatory-grade compliance | Variable | Required |
A video call lets a doctor see a patient. A clinical teleconsultation lets a doctor examine one.
The Core Components of a Clinical Teleconsultation
For a teleconsultation to meet clinical standards, several things need to work together inside a single workflow. When any one component is missing or disconnected, the clinical value degrades.
1. Real-Time Device Integration
This is the defining feature — the thing that separates clinical teleconsultation from everything else. The remote clinician needs access to objective physiological data, not just what the patient or local nurse describes, but what the instruments actually measure.
That means hardware like 12-lead ECG machines, digital stethoscopes, pulse oximeters, and blood pressure monitors needs to transmit data live into the consultation. The remote doctor should be able to hear heart sounds, review an ECG trace, and see vital signs in real time — all linked directly to the patient file.
Without this, the clinician is working with incomplete information. And decisions made on incomplete information carry both clinical and legal risk.
2. Secure, High-Quality Video
The video layer needs to be reliable enough for clinical use. Dropped frames during auscultation or a frozen screen during a neurological assessment aren't just inconvenient — they compromise the consultation. Healthcare-grade video infrastructure also has to meet data protection requirements that consumer tools typically don't.
3. Structured Clinical Documentation
Every clinical encounter needs a record. In a teleconsultation, documentation matters even more because the consulting clinician isn't physically present — the local nurse or health worker may be the one with hands on the patient.
AI-assisted transcription and automatic SOAP note generation — covering Subjective, Objective, Assessment, and Plan — significantly reduce administrative burden and the risk of incomplete records. When device data is automatically uploaded to the patient file alongside the note, the record is complete without any manual data entry.
4. Specialist Referral Capability
Many teleconsultations exist precisely because specialist access is limited. A primary care doctor or nurse should be able to escalate to a specialist within the same platform — sharing the patient record, device data, and consultation notes without re-entering anything or switching systems.
This tele-expertise function is what makes teleconsultation a genuine care pathway rather than a one-off event.
5. Scheduling, Billing, and Workflow
A clinically excellent teleconsultation that can't be scheduled, billed, or tracked isn't a sustainable healthcare service. Integrated scheduling and billing are operational requirements, not optional extras.
Who Uses Clinical Teleconsultation — and Why
The use cases are broad, but they share a common thread: distance or access constraints that make in-person specialist care impractical.
Primary Care Networks
GPs and primary care nurses use teleconsultation to access specialist opinion without sending patients out of the network. A GP can run a cardiology teleconsultation with a live ECG transmission, get a specialist read, and manage the patient locally — cutting unnecessary hospital referrals and reducing wait times.
Nursing Homes and Long-Term Care
Elderly residents often have multiple comorbidities and frequent clinical needs, but regular specialist visits are logistically difficult. Teleconsultation lets an on-site nurse conduct a medically valid consultation with a remote physician — capturing vitals, ECG, and auscultation data — without transporting a frail patient.
Rural and Remote Health Services
Distance is the original driver of telemedicine. In rural areas, clinical teleconsultation gives local health workers access to diagnostic support that would otherwise require hours of travel. Mobile configurations — including backpack-format hardware kits — make it possible to bring the consultation to the patient rather than the other way around.
Health Ministries and International Health Programs
Large-scale deployments — national telehealth programs, humanitarian health missions, occupational health services for distributed workforces — require platforms that operate across multiple languages, comply with different national regulatory frameworks, and can deploy either in the cloud or fully on-premise depending on data sovereignty requirements.
Occupational Health
Companies with large or geographically dispersed workforces increasingly use teleconsultation for occupational health assessments, follow-up consultations, and fitness-for-work evaluations. The ability to conduct a clinically valid examination remotely — including cardiac assessment — makes teleconsultation viable for contexts where it simply wasn't before.
What a Clinical Teleconsultation Platform Needs to Do
When evaluating platforms, the feature list matters less than whether the platform handles the full clinical workflow without forcing clinicians to work around it.
Here's what a serious platform needs to cover:
Device connectivity. ECG machines, digital stethoscopes, dermatoscopes, and other clinical hardware should connect directly to the platform and push data automatically to the patient record. Manual entry between device and record is a point of failure.
Patient record management. The platform should create, update, and retrieve patient records within the consultation workflow — not as a separate step in a separate system.
AI-assisted documentation. Real-time transcription and automatic SOAP note generation reduce documentation time and improve record completeness. Multilingual support matters for international deployments.
Tele-expertise and referral. Specialist referral should happen within the platform, with the full patient record and device data shared automatically.
Scheduling and billing. These aren't peripheral features. They determine whether the service is operationally viable.
Compliance and deployment flexibility. HIPAA, GDPR, and equivalent national frameworks are non-negotiable. Cloud SaaS works for many providers; fully on-premise deployment is required for others, particularly in public health and government contexts.
Implementation speed. A platform that takes six months to deploy is a barrier to adoption. Healthcare providers need solutions that are operational in weeks, not quarters.
Common Misconceptions About Clinical Teleconsultation
"It's just a video call with a doctor."
This is the most common misunderstanding. A video call is a communication tool. A clinical teleconsultation is a structured clinical encounter with device data, documented findings, and a care pathway. The difference is clinically and legally significant.
"The technology is too complex for routine use."
Modern platforms are built for clinical staff, not IT specialists. A nurse should be able to set up a consultation, connect a device, and transmit data without technical support. If the platform requires significant training or technical intervention for routine use, it isn't fit for purpose.
"Teleconsultation can't replace physical examination."
For some clinical scenarios, that's true. But for a significant proportion of consultations — follow-ups, chronic disease management, cardiology screening, respiratory assessment — hardware-integrated teleconsultation captures the same objective data an in-person visit would. The question isn't whether it's identical to in-person care, but whether it's clinically sufficient for the specific encounter.
"Data security is a bigger risk remotely."
A properly certified teleconsultation platform with end-to-end encryption, access controls, and audit logging can be more secure than a paper-based or fragmented local system. The risk isn't in the technology — it's in choosing platforms that haven't been built to clinical data standards.
How MedConnect Approaches Clinical Teleconsultation
MedConnect was built specifically for this problem. The platform connects clinical hardware — ECG machines, digital stethoscopes, vital sign monitors — directly to a patient file in real time, so the remote doctor receives the same objective data they would have in person.
A 12-lead ECG, for example, is automatically uploaded as a PDF to the patient record within five seconds of acquisition, with no manual data entry required. The remote clinician sees the trace live during the consultation and has it permanently documented without any additional steps.
The AI medical scribe transcribes the consultation in real time and generates a SOAP note automatically — in English, French, Arabic, or Italian. The Elara AI clinical assistant handles patient record creation, availability checks, and drug database queries through natural language, reducing administrative overhead during and after the consultation.
When specialist input is needed, the tele-expertise module allows referral within the same platform. The specialist receives the full patient record and all device data without the referring clinician needing to export, email, or re-enter anything.
MedConnect deploys in two to four weeks as cloud SaaS or fully on-premise, with data center options in the US, EU, and Middle East. It carries compliance certifications for global use — which matters for health ministries and international organizations operating across multiple regulatory environments.
Hardware configurations include a medical kit, a cart, and a backpack, all connecting to the same platform. The backpack format is particularly relevant for mobile health programs and remote deployments where bringing equipment to the patient is the only practical option.
Evaluating Your Options: What to Ask
Whether you're a primary care network, nursing home operator, or health ministry assessing teleconsultation platforms, these are the questions that actually matter:
- Does the platform integrate directly with clinical hardware, or does device data require manual entry? Manual entry is both a clinical risk and an operational bottleneck.
- Is documentation automated, or does the clinician write notes separately? AI-assisted SOAP note generation is now standard in serious platforms.
- Can specialist referral happen within the platform? If not, you're building a workflow with gaps.
- What are the deployment options? Cloud-only platforms may not meet data sovereignty requirements in certain jurisdictions.
- How long does implementation take? Anything beyond four to six weeks deserves scrutiny.
- What compliance certifications does the platform hold? HIPAA, GDPR, and relevant national certifications are baseline requirements.
- Is the platform multilingual? For any international or multicultural deployment, this isn't optional.
- What does the hardware ecosystem look like? A platform that only works with one proprietary device limits your flexibility.
The Direction of Travel
Clinical teleconsultation isn't a pandemic-era workaround. It's a structural shift in how healthcare is delivered — driven by demographic pressure, specialist shortages, the geographic distribution of populations, and the maturation of the underlying technology.
The platforms that will define this space aren't the ones with the best video quality. They're the ones that handle the full clinical encounter: device data, documentation, referral, billing, and compliance — in a single workflow that clinicians can actually use without friction.
The gap between a video call and a clinical teleconsultation is the gap between talking about care and delivering it.
Conclusion
Clinical teleconsultation is a structured, device-integrated, documented clinical encounter conducted remotely. It isn't a synonym for telemedicine, and it isn't a video call. When it works properly, it gives a remote clinician the same diagnostic information they would have in person — and produces a complete clinical record without additional manual steps.
For primary care networks, nursing homes, rural health services, and large-scale health programs, it represents a practical answer to access constraints that aren't going away.
The technology to do this well exists. The question for healthcare providers is whether the platform they choose actually delivers the full clinical workflow — or just the video layer.
Learn more at promotal-medconnect.com
Ready to discover MedConnect?
Request a personalized demo and see how the platform adapts to your practice.
Request a demo