Digital Stethoscope Telemedicine: How Remote Auscultation Works in Clinical Practice
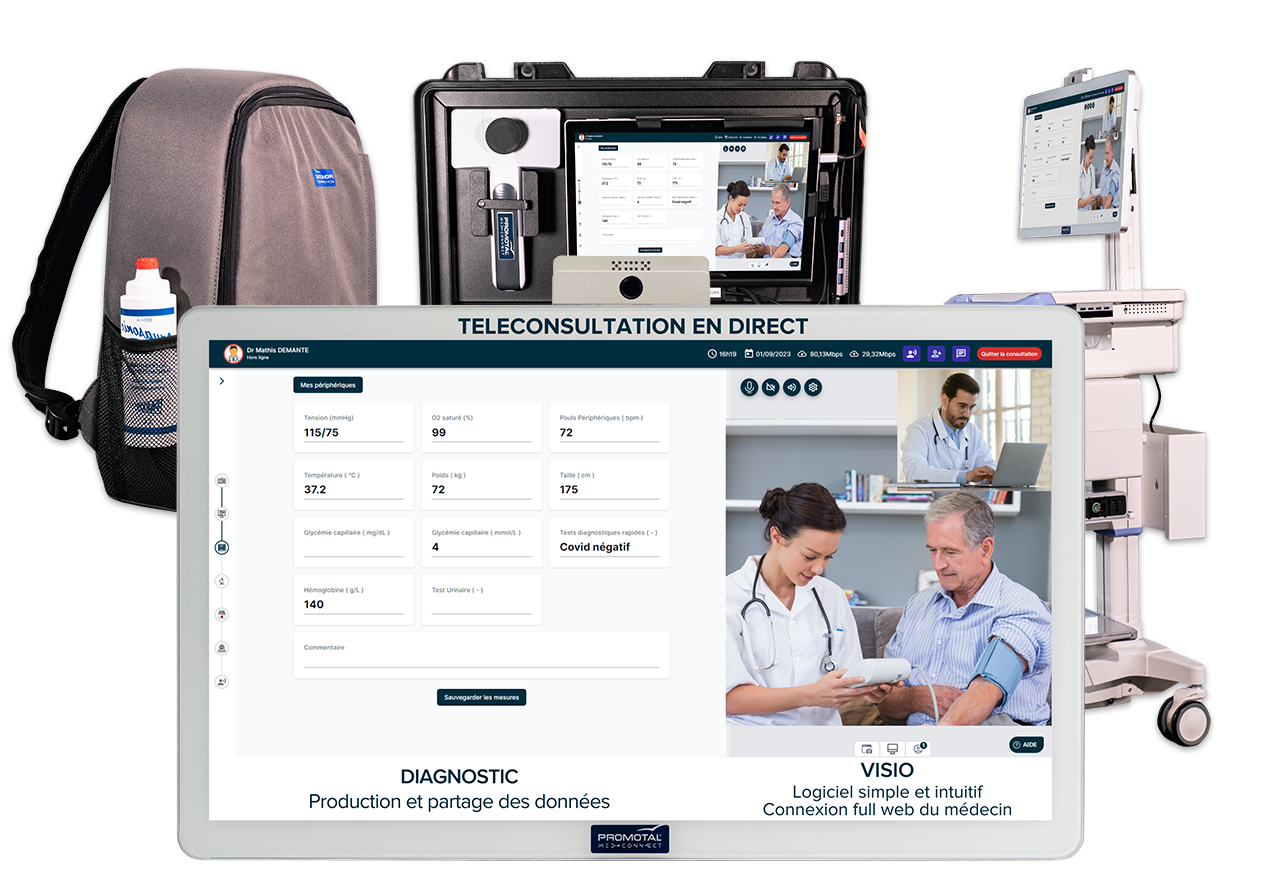
The Clinical Reality of Remote Auscultation
A 68-year-old patient presents with chest discomfort at a rural nursing facility. The on-site nurse needs immediate cardiac assessment, but the nearest cardiologist is 90 minutes away. Traditional telemedicine offers video consultation. Digital stethoscope telemedicine delivers real-time auscultation data directly to the specialist's screen.
This distinction matters. Remote auscultation through digital stethoscopes transforms teleconsultation from symptom discussion to actual clinical examination. Heart sounds, lung patterns, and murmur detection happen in real-time, not through patient description or delayed audio files.
Digital stethoscope integration addresses a fundamental limitation in telemedicine: the inability to perform physical examination remotely. While video calls handle visual assessment and patient history, auscultation requires direct sound transmission with clinical-grade audio quality.
How Digital Stethoscopes Enable Remote Clinical Examination
Real-Time Audio Streaming Architecture
Digital stethoscopes capture cardiac and pulmonary sounds through electronic sensors, converting acoustic data into digital signals. These devices connect to telemedicine platforms via Bluetooth or USB, streaming live audio to remote physicians during consultation.
The technical foundation requires:
- High-fidelity audio capture: 20Hz to 20kHz frequency range covering heart sounds (20-200Hz) and lung sounds (100-1000Hz)
- Low-latency transmission: Sub-200ms delay for real-time clinical assessment
- Noise cancellation: Electronic filtering of ambient sounds and movement artifacts
- Signal amplification: 5x to 100x amplification for detecting subtle murmurs or abnormal sounds
Clinical Data Integration During Teleconsultation
Modern digital stethoscope telemedicine platforms integrate auscultation data directly into the clinical workflow. The examining nurse places the stethoscope on specific anatomical locations while the remote physician listens through professional-grade headphones.
Key integration points include:
- Live audio streaming during video consultation
- Recording capability for specialist review and documentation
- Waveform visualization showing sound patterns on screen
- Automatic documentation of auscultation findings in patient records
This integration eliminates the disconnect between physical examination and remote consultation. The specialist hears actual heart sounds, not descriptions of heart sounds.
Clinical Applications in Primary Care and Specialist Referral
Cardiac Auscultation in Telemedicine
Digital stethoscope telemedicine proves most valuable in cardiac assessment. Heart murmurs, irregular rhythms, and gallop sounds require direct auscultation for accurate diagnosis.
Murmur Classification: Specialists can grade murmur intensity (1-6 scale), identify timing (systolic vs. diastolic), and determine clinical significance without in-person examination.
Rhythm Assessment: Irregular heartbeats, extra sounds, and rate variations are detectable through high-quality digital transmission.
Post-Surgical Monitoring: Patients with cardiac procedures require ongoing auscultation monitoring. Digital stethoscopes enable remote follow-up without hospital visits.
Pulmonary Assessment Through Remote Auscultation
Lung sound assessment through digital stethoscopes supports respiratory condition management. Crackles, wheezes, and diminished breath sounds are identifiable through remote examination.
COPD Management: Regular lung sound monitoring helps track disease progression and medication effectiveness.
Pneumonia Detection: Early identification of abnormal lung sounds supports timely antibiotic intervention.
Asthma Monitoring: Wheeze detection and breath sound quality assessment guide treatment adjustments.
Pediatric Applications
Digital stethoscope telemedicine addresses unique pediatric challenges. Children often resist examination, making efficient auscultation essential. Remote specialists can guide local nurses through systematic examination while maintaining child comfort.
- Reduced examination time through specialist guidance
- Improved cooperation by minimizing stranger interaction
- Better sound quality through electronic amplification for small chest cavities
Technical Considerations for Clinical Implementation
Audio Quality Requirements
Clinical-grade auscultation demands specific technical standards. Consumer-grade audio equipment cannot meet diagnostic requirements for heart murmur detection or subtle lung sound identification.
Frequency Response: Digital stethoscopes must capture the full range of physiological sounds. Heart sounds occur primarily between 20-200Hz, while lung sounds span 100-1000Hz. Standard telephone audio (300-3400Hz) misses critical low-frequency cardiac information.
Dynamic Range: Heart sounds vary from barely audible S4 gallops to loud systolic murmurs. Digital stethoscopes require 60dB+ dynamic range to capture this variation without distortion.
Signal-to-Noise Ratio: Clinical assessment requires 40dB+ SNR to distinguish pathological sounds from background noise.
Platform Integration Challenges
Digital stethoscope telemedicine requires seamless integration between hardware, software, and clinical workflows. Technical challenges include:
Device Compatibility: Multiple stethoscope manufacturers (Welch Allyn, MIR, Littmann) use different connection protocols and audio formats.
Network Requirements: Real-time audio streaming requires stable internet with 1Mbps+ bandwidth and consistent latency.
Documentation Integration: Auscultation findings must integrate with electronic health records without manual data entry.
Multi-Device Coordination: Platforms must simultaneously handle video, audio, and device data streams during consultation.
Quality Assurance and Clinical Validation
Diagnostic Accuracy in Remote Auscultation
Clinical studies demonstrate digital stethoscope telemedicine maintains diagnostic accuracy comparable to in-person examination. Research shows:
- Heart murmur detection: 95%+ sensitivity for clinically significant murmurs
- Rhythm abnormality identification: 98% accuracy for atrial fibrillation detection
- Lung sound classification: 90%+ accuracy for crackles and wheeze identification
These accuracy rates depend on proper technique, quality equipment, and trained operators.
Training Requirements for Clinical Staff
Effective digital stethoscope telemedicine requires specific training for both local and remote clinical staff. On-site nurses must understand proper stethoscope placement, optimal positioning for sound transmission, and troubleshooting connection issues.
Training programs should include:
- Anatomical positioning for optimal sound capture
- Technical troubleshooting for connection and audio issues
- Artifact recognition to distinguish equipment noise from pathological sounds
- Documentation standards for remote auscultation findings
Regulatory Compliance and Security Considerations
Medical Device Regulations
Digital stethoscopes used in telemedicine must meet medical device regulations in their deployment regions. FDA Class II classification in the United States requires 510(k) clearance. European CE marking under MDR ensures safety and performance standards.
- Device validation for intended clinical use
- Software verification for diagnostic accuracy
- Risk management according to ISO 14971 standards
- Clinical evaluation demonstrating safety and effectiveness
Data Security in Remote Auscultation
Patient auscultation data requires protection under healthcare privacy regulations. HIPAA compliance in the US and GDPR compliance in Europe mandate specific security measures.
Encryption Requirements: Audio data transmission requires AES-256 encryption with TLS 1.3 protocols.
Access Controls: Role-based permissions ensure only authorized clinicians access patient auscultation data.
Audit Trails: Complete logging of device access, data transmission, and clinical documentation.
Integration with Complete Clinical Workflows
Beyond Isolated Device Data
Digital stethoscope telemedicine reaches full potential when integrated into comprehensive clinical platforms. Isolated audio transmission provides limited value compared to complete examination workflows.
Integrated platforms combine:
- Video consultation for visual assessment and patient interaction
- Digital stethoscope data for cardiac and pulmonary examination
- Vital signs monitoring for blood pressure, temperature, and oxygen saturation
- ECG integration for cardiac rhythm analysis
- Electronic health records for complete documentation
Real-World Implementation Example
Consider a primary care network implementing digital stethoscope telemedicine across 25 rural clinics. Each site has trained nurses using integrated telemedicine platforms that combine video consultation with medical device data.
During a typical consultation:
- Patient check-in through the platform scheduling system
- Vital signs collection automatically uploaded to patient record
- Video consultation initiated with remote physician
- Digital auscultation performed with live audio streaming
- ECG capture if indicated, with automatic interpretation
- Clinical documentation generated through AI assistance
- Specialist referral processed within the same platform if needed
Measuring Clinical Impact and ROI
Clinical Outcome Metrics
Successful digital stethoscope telemedicine implementation shows measurable clinical improvements:
Diagnostic Accuracy: Comparison of remote vs. in-person auscultation findings
Time to Diagnosis: Reduction in specialist referral delays
Patient Satisfaction: Comfort with remote examination quality
Clinical Confidence: Provider satisfaction with diagnostic information quality
Operational Efficiency Gains
Digital stethoscope integration delivers operational benefits beyond clinical outcomes:
Reduced Travel: Patients avoid specialist visits for routine auscultation
Faster Consultations: Real-time examination vs. appointment scheduling delays
Documentation Efficiency: Automated recording and transcription of findings
Specialist Utilization: More patients seen through remote consultation capacity
Healthcare organizations typically see 40-60% reduction in unnecessary specialist referrals and 25-30% improvement in diagnostic turnaround times.
Future Developments in Remote Auscultation Technology
AI-Enhanced Sound Analysis
Machine learning algorithms increasingly support digital stethoscope interpretation. AI systems can identify abnormal heart sounds, classify murmur types, and flag urgent findings for immediate physician review.
- Automated murmur detection with 95%+ sensitivity
- Heart rate variability analysis for arrhythmia screening
- Lung sound classification for respiratory condition monitoring
- Trend analysis comparing patient sounds over time
Conclusion
Digital stethoscope telemedicine transforms remote consultation from symptom discussion to actual clinical examination. Real-time auscultation data enables accurate cardiac and pulmonary assessment without in-person visits.
Success requires more than connecting a digital stethoscope to video calls. Effective implementation demands clinical-grade audio quality, seamless workflow integration, comprehensive training, and robust security measures.
Healthcare organizations implementing digital stethoscope telemedicine as part of complete clinical platforms see the greatest impact. Integrated systems that combine video, devices, records, and billing deliver operational efficiency alongside improved clinical outcomes.
Learn more at promotal-medconnect.com
Ready to discover MedConnect?
Request a personalized demo and see how the platform adapts to your practice.
Request a demo